Keratoconus Treatment
What is Keratoconus?
Keratoconus means “conical or cone-shaped cornea”. It is a condition where the cornea (the clear window on the front of the eye) becomes stretched and thin and begins to bulge into a cone-like shape. Because the cornea is the major focussing surface of the eye, this causes blurred and distorted vision.
In keratoconus the normal physical properties of the cornea are altered, and this causes refractive error, usually short-sightedness (myopia) and irregular high astigmatism. It can be iatrogenic (called keratectasia or corneal ectasia), for example, following laser-in-situ keratomileusis (LASIK).
Diagnosis of keratoconus is based on corneal thinning at the apex of the corneal cone (found on slit-lamp examination) and corneal topographic and keratometric assessment of the curvature of the cornea. Keratoconus commonly affects children and young adults. The stretching of the cornea tends to progress but the rate varies. It usually affects both eyes, but sometimes one eye may be badly affected whilst the other eye shows very little sign of the condition.
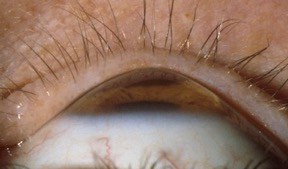
What are the symptoms of keratoconus?
Keratoconus leads to increasing astigmatism in the glasses prescription, and the glasses prescription is not stable. Although some people with early keratoconus may be able to wear spectacles or soft contact lenses, when keratoconus becomes more severe, glasses are unable to give sharp vision because of irregular astigmatism. With irregular astigmatism, gas permeable contact lenses give best vision.
What can happen if keratoconus is not treated?
If keratoconus is not treated, as the disease progresses, gas permeable contact lenses are not sufficient to correct visual acuity, or cannot be tolerated due to poor fit as a consequence of the abnormal corneal shape. Intracorneal ring segment implants (e.g. Keraring, Intacs) may be used. Deep lamellar keratoplasty or penetrating keratoplasty may be required for severe progressive keratoconus.
Hydrops is a condition encountered in severe keratoconus, where the thin membrane at the back of the cornea (Descement’s membrane) spontaneously ruptures as the cornea becomes more cone shaped. Vision is compromised initially with hydrops, but over time the vision usually recovers to previous levels. Sometimes vision can recover to a better level following hydrops, due to flattening of the cone shape during healing.
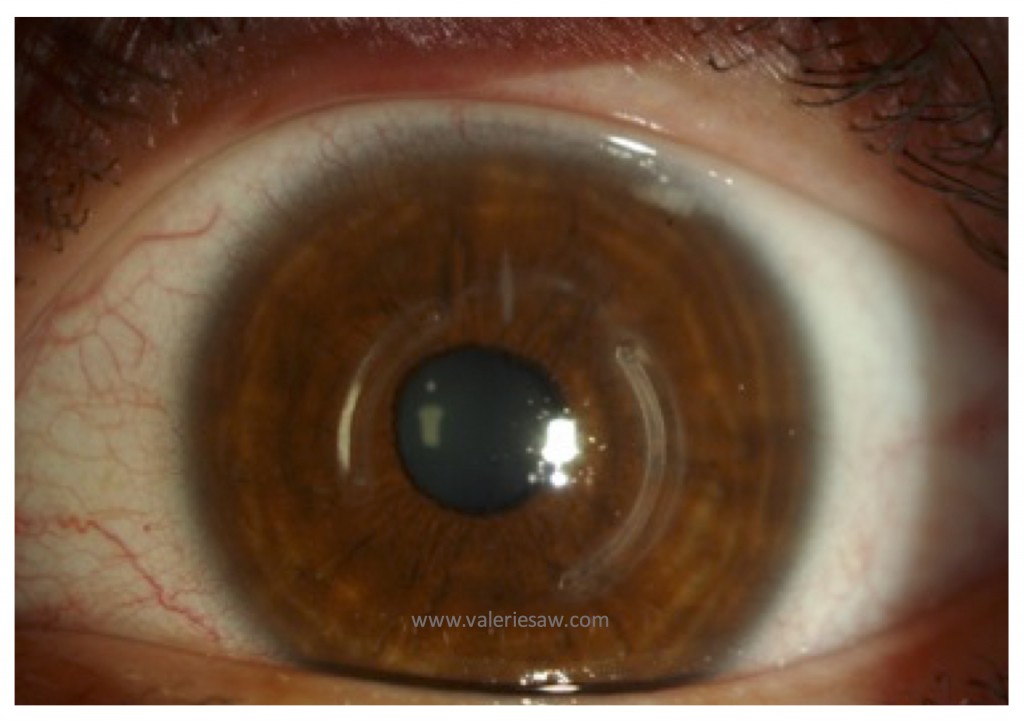
How is keratoconus diagnosed?
Keratoconus is diagnosed by a combination of:
- An abnormal corneal topography scan such as Pentacam, and
- Increasing astigmatism in the glasses prescription.
What treatments are available for keratoconus?
Collagen cross-linking has been shown in several randomized trials to halt the progression of keratoconus. Cross-linking is the currently the only treatment available, which halts the progression of keratoconus.
Intracornal ring segments can improve vision in keratoconus. Ring segments can be used in patients who would like a better shape of the cornea, to allow soft contact lens wear or glasses, and avoid having a corneal transplant.
Surface laser reshaping combined with collagen cross-linking treatment shows promise in improving the corneal shape and reducing the irregularity of astigmatism in mild to moderate keratoconus, allowing patients to wear glasses or soft contact lenses and avoid having a corneal transplant.
Corneal transplantation, most commonly deep anterior lamellar keratoplasty, to remove the abnormal thinned cornea, is the final treatment option.
Why choose Miss Saw for your keratoconus treatment?
Valerie Saw is an expert consultant ophthalmic surgeon and an outstanding surgeon. As a Member of the Council of the British Society of Refractive Surgeons, and an invited Examiner for the Royal College of Ophthalmologists’ Certificate for Laser Refractive Surgery in the UK, she is recognized by her peers for her expertise in cornea, lens and laser eye surgery. She has been voted amongst the top 10 Laser Eye Surgeons in the UK by patients, for her outstanding surgical skills.

Don't take our word for it
Reviews from happy patients
Message Us
Get In touch below. Ask Any Questions or Start a Free Quote
Call Us
0203 328 0076
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
Clinic Address
The London Clinic 119 Harley Street London W1G 6AU
Open Hours
pm@valeriesaw.com